Biomarkers for Stroke
Article information
Abstract
Background
Major stroke clinical trials have failed during the past decades. The failures suggest the presence of heterogeneity among stroke patients. Biomarkers refer to indicators found in the blood, other body fluids or tissues that predicts physiologic or disease states, increased disease risk, or pharmacologic responses to a therapeutic intervention. Stroke biomarkers could be used as a guiding tool for more effective personalized therapy.
Main Contents
Three aspects of stroke biomarkers are explored in detail. First, the possible role of biomarkers in patients with stroke is discussed. Second, the limitations of conventional biomarkers (especially protein biomarkers) in the area of stroke research are presented with the reasons. Lastly, various types of biomarkers including traditional and novel genetic, microvesicle, and metabolomics-associated biomarkers are introduced with their advantages and disadvantages. We especially focus on the importance of comprehensive approaches using a variety of stroke biomarkers.
Conclusion
Although biomarkers are not recommended in practice guidelines for use in the diagnosis or treatment of stroke, many efforts have been made to overcome the limitations of biomarkers. The studies reviewed herein suggest that comprehensive analysis of different types of stroke biomarkers will improve the understanding of individual pathophysiologies and further promote the development of screening tools for of high-risk patients, and predicting models of stroke outcome and rational stroke therapy tailored to the characteristics of each case.
Discovering biomarkers for stroke
In a narrow sense, biomarkers refer to indicators measured by chemical or biologic tests using blood or urine that predicts physiologic or disease states, or increased disease risk. Biomarkers are also a valuable tool in drug development, providing more accurate and complete information regarding drug performance, disease progression, or response to a specific drug therapy. In the research field of myocardial infarction, the role of biomarkers has been emphasized over a long period of time. Treatment according to the biomarkers has also been investigated in various diseases including diabetes or immunological disorders. On the contrary, there has been a relative dearth of biomarker research in cerebrovascular disease. Herein, we review the role of current and new stroke biomarkers with their strengths and weaknesses, focusing on the importance of comprehensive approaches.
Learning from the failure of recent clinical trials
Over the recent 10 years, numerous large multicenter randomized clinical trials (RCTs) on stroke patients have been performed in the stroke research field. However, almost all major studies including RCTs regarding secondary prevention of stroke,1-3 MR-based thrombolytic therapy,4,5 and STAIR (Stroke Treatment Academic Industry Roundtable) criteria-guided neuroprotection6 have failed to show meaningful clinical benefits. In this regard, several issues have been suggested to explain and overcome these failures.
First, it is warranted for more larger and methodologically sound RCTs which meet the STAIR7 and CONSORT8 (CON-solidated Standards Of Reporting Trials) criteria. These may enhance the success rate and reliability of the study. It is clear that findings derived from large-scale intervention trials have provided the impetus to change guidelines for stroke treatment. Nonetheless, direct application of RCTs results to daily clinical practice is dubious, because patients enrolled in large RCTs may not be representative of patients in our clinical practice.9
Second, there has been increasing interest in new statistical approaches to end-point analysis in RCTs (from dichotomized outcome scales to global statistics, responder, or shift analysis).10 These are mainly used to reduce sample size or enhance trial efficiency.11 Unfortunately, however, researchers cannot draw any new findings from RCTs through the novel statistical methods.
Third, the importance of considering heterogeneity among stroke patients has emerged. Unlike coronary heart disease, stroke has heterogeneous pathophysiologies and mechanisms. Moreover, individual patients with stroke have different features even among subjects with same stroke mechanisms. These aspects enhance the need for development of personalized medicine based on the characteristics of each patient rather than performing large RCTs. Stroke biomarkers may provide the information on the heterogeneity and could be a guiding tool for more effective personalized therapy among patients with ischemic cerebrovascular disease.
Role of biomarkers in stroke research
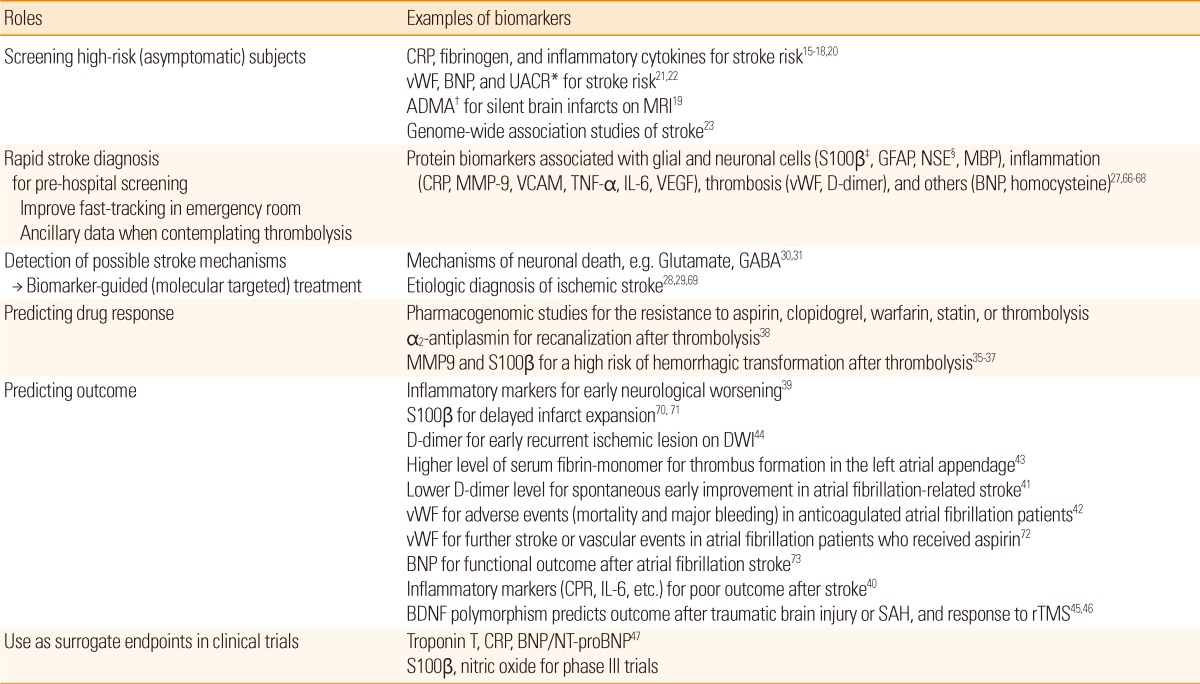
Emerging roles of stroke biomarkers are summarized in Table 1. Although the roles of biomarkers are basically diagnosing the disease and predicting the outcome, biomarkers in patients with stroke can also provide a large variety of other information about the risk of future stroke, possible stroke mechanisms for biomarker-guided treatment, or drug response. In addition, they can be used as surrogate endpoints in clinical trials.
Screening high-risk subjects
Although many attempts, including national publicity and various programs for health promotion, have been made to manage stroke risk factors, the prevalence of stroke has not been markedly reduced. This may be partially attributable to hidden risk factors of stroke. Interestingly, certain regions in the United States (Stroke Belt and Buckle) have an unusually high incidence and mortality of stroke and the phenomenon could not be explained by the differences of the conventional risk factors.12,13 The exact causes of the higher incidence and mortality of stroke in the regions have not been recognized. Therefore, many researchers have devoted themselves to find novel risk factors of stroke to explain it, whereupon numerous possible contributing factors have been identified, including obesity/metabolic syndrome, diet, sleep-related breathing disorders, air pollution, and cultural lifestyle.14
In addition to finding these new risk factors, a series of biomarkers reflecting inflammation, hemostasis, thrombosis, endothelial function, or neurohormonal activity have been evaluated as potential tools in an effort to improve risk prediction of future stroke, and thereby avert future events.15-22 For example, a recent investigation using data from the Framingham offspring study found that plasma asymmetrical dimethylarginine (ADMA) which is an inhibitor of endothelial nitric oxide synthase (eNOS) and a marker of endothelial dysfunction was associated with a prevalence of silent brain infarcts which is an important correlate of risk of future stroke.19 More recently, the same group published data on multiple biomarkers and identified that baseline B-type natriuretic peptide (BNP) having diuretic and vasodilatory activities and a urinary albumin/creatinine ratio indicating endothelial function were associated with the risk of incident stroke, and offered modest improvements in the accuracy of risk stratification.22 In the near future, a genome-wide association study may also greatly contribute to building risk stratification models by identifying genetic variants that confer susceptibility to cerebrovascular disease.23
Rapid stroke diagnosis
Although the diagnosis of acute stroke mostly relies on neuroimaging techniques, the evaluation of biomarkers of tissue injury would be an alternative strategy for rapid stroke assessment. This approach has already been successfully applied in the early management of other diseases including coronary heart disease (troponin, CK-MB), pulmonary embolism (D-dimer), and congestive heart failure (BNP).24-26 A rapid diagnosis of stroke based on biomarkers may be useful especially for pre-hospital screening, facilitating entry into a fast track care pathway, and for ancillary data when contemplating thrombolysis. However, a widely available, rapid, and sensitive diagnostic test for acute cerebral ischemia has not been available until now.
Recently, a biomarker panel rather than a single marker in isolation has been increasingly used to improve the diagnostic accuracy of suspected stroke. For instance, a diagnostic panel incorporating the levels of matrix metalloproteinase 9 (MMP-9), BNP, D-dimer, and S-100β into a composite score enhanced sensitivity of early noncontrast CT alone for acute stroke, although the diagnostic accuracy was clearly imperfect.27 Furthermore, the approach was feasible as a point-of-care test in the emergency setting.27 As the number of presumed biomarkers for stroke expands at an exponential rate, it would be expected to develop improved biomarker combinations for more accurate diagnosis of stroke.
Detection of possible stroke mechanisms
Several studies have focused on the use of biomarkers for detecting possible stroke mechanisms. A recent study investigated whether concentrations of von Willebrand factor (vWF) which plays crucial roles in thrombus formation differ depending on the etiologic subtypes of stroke, and found the highest levels in large artery disease and cardioembolic stroke.28 Recent data by our group also demonstrated that inflammatory markers, rather than traditional risk factors were associated with clinical and radiological differences among patients with atherosclerotic stroke.29 In addition, the molecular markers related to neuronal death can provide information about the presence of tissue at risk of infarction.30,31
Predicting drug response and outcome
It has been well known that different patients respond in different manners to the same medication. Among many factors that influence the effects of drugs, it is estimated that genetic factors can account for 20 to 95% of variability in drug disposition and effects.32 For example, previous studies revealed that CYP2C9 and VKORC1 genetic variants are associated with warfarin dose requirement and clinical outcomes.33,34 Besides pharmacogenetics, several biomarkers are also contributing to predicting drug responses in patients with stroke, particularly when thrombolysis is administered. Specifically, elevated S-100β and MMP-9 which were reported as serum markers of blood-brain barrier (BBB) dysfunction before thrombolysis could predict hemorrhagic transformation after thrombolysis,35-37 whereas baseline levels of α2-antiplasmin were predictive of recanalization in patients treated with rt-PA.38
There has been mounting evidence that a number of biomarkers can predict clinical or radiological outcomes from cerebral ischemic events. Inflammatory markers such as C-reactive protein (CRP) or proinflammatory cytokines are reportedly associated with early neurological worsening or poor functional outcome after stroke.39,40 Biomarkers related to coagulation/fibrinolysis system such as D-dimer or vWF may also have links with outcome prediction, especially in patients with cardioembolic stroke.41-44 Very recently, it was reported that genetic polymorphisms of brain-derived neurotrophic factor (BDNF) was associated with functional outcome after subarachnoid hemorrhage, and cortical plasticity.45,46
Surrogate endpoints in clinical trials
In cardiovascular diseases, many investigators have used biomarkers that correlate with clinical outcomes as surrogate endpoints, because event-driven clinical trials require much of the cost and time burden.47 In the area of stroke research, several studies has been started to use biomarkers to monitor the efficacy and safety of treatments in phase III clinical trials. However, changes detected in surrogate markers do not always translate into clinical endpoints, and may even be the opposite with clinical outcomes.48 Thus, biomarkers may be useful as a screening tool and secondary outcomes, but not primary outcome in clinical trials at the present time.
Type of biomarkers in stroke research
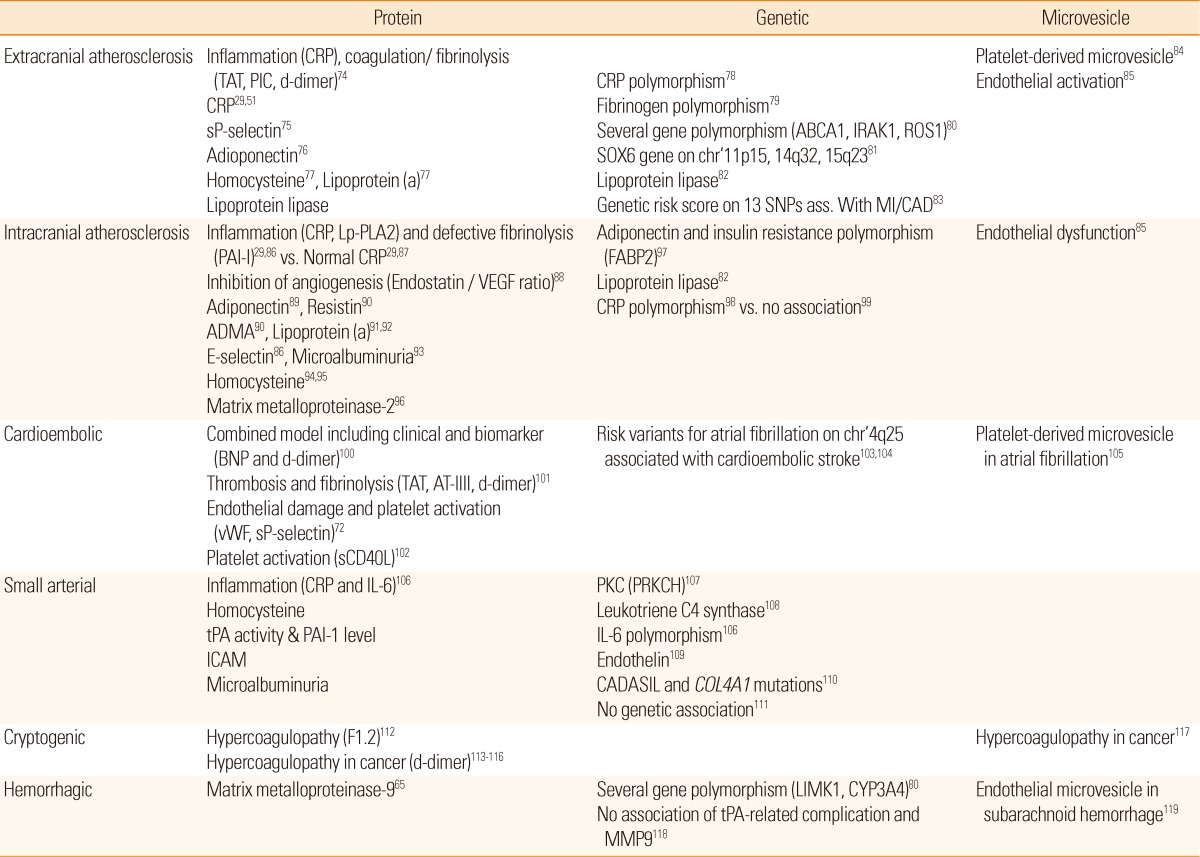
Stroke biomarkers include traditional protein biomarkers and novel genetic, microvesicle, and metabolomics-associated biomarkers (Table 2).
Protein biomarkers
Research using protein biomarkers in patients with ischemic cerebrovascular disease have mainly focused on pathophysiology, diagnosis, prognostication, and neuronal death in stroke.49 A typical example of protein biomarkers is CRP.17,50,51 However, a recent study raised the possibility that the relation may result from various biases.52 Moreover, it has raised skepticism about the efficacy of biomarkers in predicting stroke risk because they provide only limited additional information compared to the well-known stroke risk factors.53,54 Further studies with more a systematic approach and analysis are needed in this area.
Genetic biomarkers
Many epidemiological studies suggested that stroke has genetic susceptibility, and various genetic factors were investigated.55 Among them, establishing the association of the 9p21.3 locus with risk of cerebral infarction is one of the biggest advances.56 It is estimated that the genetic influence is caused by enhanced platelet reactivity.56 However, many other genome-wide association studies failed to reproduce the positive results obtained from previous studies57 or have shown that the clinical usefulness was very low.58 For example, the hazard ratio and population attributable risk of hypertension to ischemic stroke is 2.0 and 26%, respectively. Conversely, the genetic influence on stroke was only 1.3-1.33 and 11-12%, respectively.58
Recently, studies in the pharmacogenomic area have been actively carried out. Among them, aspirin, clopidogrel, warfarin, statin, and thrombolytics-related genetic polymorphisms are particularly of interest. It is expected that selecting the type or dose of medication, avoiding side effects, or drug resistance may be guided by simple genetic tests in the near future.
Microvesicle
Microvesicles are defined as a heterogeneous population of small vesicles with a diameter of 0.1-1 µm. It was previously believed that microvesicles were artifacts generated by apoptotic cell death. However, this view has changed because the shedding of these small vesicles was recognized to result from an active process.59 Microvesicles may be a window for target cell/organs, and include genetic information as well as protein inside them.60 Moreover, it has been identified that microvesicles have their own function, revealing that microvesicles from ischemic tissue facilitated vasculogenesis in the ischemic limb model.61 In this regard, biomarker research using microvesicles is a prominent field.
Nevertheless, biomarker studies using microvesicles in stroke are mostly performed in small cohorts. As the methods for analyzing microvesicles are complicated and not unique mainly due to their very small size, investigations with microvesicles are currently at a rudimentary state of development. When seeing the results from a large-scale clinical study perspective for the prediction of the future risk of myocardial infarction, microvesicles could be a good candidate to compensate for the limitations of existing biomarker researches.62
Metabolomics
The assumption of metabolomics is that occurrence of the disease is directly related to the specific change of biochemical composition in the cell or biological fluid. Metabolomics-associated biomarker research analyzes profiles of fatty acids, amino acids, or polyamine in the blood or urine and determines normal or pathologic states. Furthermore, metabolomics-associated biomarkers can be applied to the monitoring recovery after treatment. Unfortunately, studies using metabolomics in the area of stroke is relatively lacking.
Limitations of stroke biomarkers
Currently, the application of biomarkers in the management of cerebral infarction has some limitations, despite their evolving role.
First, unlike myocardial infarction, changes in the brain are not sufficiently reflected by blood biomarkers due to the presence of the blood-brain barrier (low sensitivity and underpowered).
Second, biomarkers can change by a variety of comorbid conditions or brain damage itself (confounders and lack of specificities). As asymptomatic coronary atherosclerosis is frequently accompanied in patients with ischemic stroke,63 it may confound the levels of biomarkers. Indeed, our group recently found that the burden of asymptomatic coronary atherosclerosis was the most important factor for levels of C-reactive protein and homocysteine, regardless of vascular risk factors and the degree and distribution of cervicocephalic atherosclerosis (Figure 1).64 Furthermore, the direct role of biomarkers in the disease process may be hard to reveal. For example, matrix metalloproteinase-9 (MMP-9) which is known as a marker of hemorrhagic transformation after thrombolysis65 is significantly associated with the size of the cerebral infarction irrespective of hemorrhagic transformation.29 Therefore, it is difficult to establish the causal relationship between biomarkers and ischemic stroke in a real clinical setting.

Distribution of CRP according to the (A) severity of cerebral atherosclerosis or (B) asymptomatic burden of coronary atherosclerosis in patients with stroke. CRP values are proportional to the increase of coronary (P=0.010 for trends), but not cerebral atherosclerosis (P=0.131 for trends). Severity of cerebral or coronary atherosclerosis. I: No atherosclerosis or 1 segment with <50% stenosis, II: ≥2 segments with <50% stenosis, III: 1 segment with ≥50% stenosis, IV: ≥2 segments with ≥50% stenosis.
Third, there is no sufficiently robust single marker for stroke. As shown in Table 2, ischemic stroke is a complex process that includes various etiologies. In addition, the brain consists of many different cells with vessels having distinct anatomical characteristics.
Future direction and summary: need of comprehensive approach
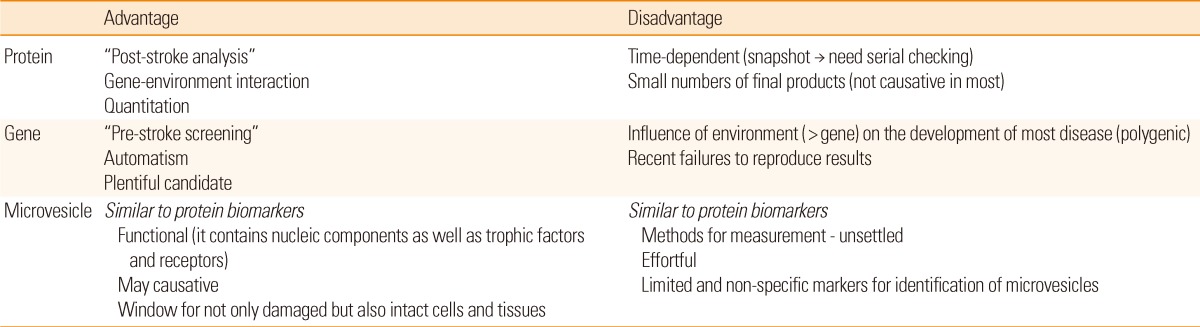
Each biomarker has different aspects, and its own advantages and drawbacks (Table 3). Therefore, developing an integrated panel of biomarkers for specific stroke subtypes is needed. A recent study reported that multiple microparticle biomarkers in addition to existing protein biomarkers are valuable for predicting future cardio- and cerebrovascular events.62 Hence, a comprehensive approach to using a variety of biomarkers is warranted to overcome the limitations. In addition, multidisciplinary approaches including neuroimaging biomarkers are needed.
A number of biomarkers are under investigation in patients with ischemic stroke. Research about biomarkers can be helpful especially in predicting stroke and monitoring therapeutic effects. Currently, however, the application of biomarkers is only recommended for research purposes. Monitoring traditional risk factors or vessel status is more efficacious than measuring biomarkers in clinical practice. Considering the advantages and disadvantages of each biomarker is important for future study, and a comprehensive approach using multiple biomarkers is needed. It is strongly anticipated that the biomarkers can provide us a turning point for investigating pathophysiology and therapeutic mechanisms of ischemic stroke.
Notes
This study was supported by the Korean Healthcare Technology R&D Project, Ministry of Health & Welfare (A110208) and the Bio & Medical Technology Developmental Program of the National Research Foundation of Korea, Ministry of Education, Science and Technology (2011-0019389).
The authors have no financial conflicts of interest.