Non-Vitamin K Oral Anticoagulants Associated Bleeding and Its Antidotes
Article information
Abstract
Oral anticoagulant-associated intracerebral hemorrhage (OAC-ICH) accounts for nearly 20% of all ICH. The number of patients with an indication for oral anticoagulant therapy (OAT) increases with increasing age. OAT became less complicate with the introduction of non-vitamin K oral anticoagulants (NOAC) OAT because of easier handling, favorable risk-benefit profile, reduced rates of ICH compared to vitamin K antagonists and no need for routine coagulation testing. Consequently, despite a better safety profile of NOAC the number of patients with OAC-ICH will increase. The mortality and complication rates of OAC-ICH are high and therefore they are the most feared complication of OAT. Immediate normalization of coagulation is the main goal and therefore knowledge of pharmacodynamics and coagulation status is essential. Laboratory measurements of anticoagulant activity in NOAC patients is challenging as specific tests are not widely available. More accessible tests such as the prothrombin time and activated partial thromboplastin time have important limitations. In dabigatran-associated ICH 5 g Idarucizumab should be administered. In rivaroxaban and apixaban-associated ICHs administration of andexanet alpha should be considered. Prothrombin complex concentrate may be considered if andexanet alpha is not available or in case of an ICH associated with edoxaban.
Introduction
Ten to 17% of all strokes are intracerebral hemorrhages (ICHs) [1]. Oral anticoagulant-associated ICH (OAC-ICH) accounts for nearly 20% of all ICH [2]. Non-valvular atrial fibrillation (NAF) is one of the most common indications for OAC and the incidence has continued to rise, because of advances in early detection and treatment [3,4]. Anticoagulants are recommended for a broad range of indications. If assuming 70% of 5 million Europeans with NAF were on OAC (approximately 40% on non-vitamin K oral anticoagulant [NOAC], and 30% on vitamin K antagonists [VKAs]) [5] and an average rate of 0.6% OAC-ICH per year, this corresponds to 21,000 cases OAC-ICH each year in Europe.
NOACs were developed to directly inhibit thrombin or factor Xa. Randomized controlled trial (RCT) data and meta-analyses provide solid evidence for a favorable risk-benefit profile of NOACs when compared with warfarin and with low-molecular-weight heparin for primary and secondary prevention in patients with NAF and treatment/prevention of venous thromboembolism, respectively [6,7]. Advantages of NOACs are easier handling, reduction in fatal and life-threatening bleeding (as ICH), and fewer drug and food interactions. For these reasons and because of current and expected approval of different reversal agents the use of NOAC will further increase [8]. Consequently, the number of patients with OAC-ICH will increase, despite the lower risk of intracranial bleeding of NOACs (compared to VKAs) [9].
The aim of this review is to address the clinical management of patients with NOAC-associated ICH.
Laboratory measurements
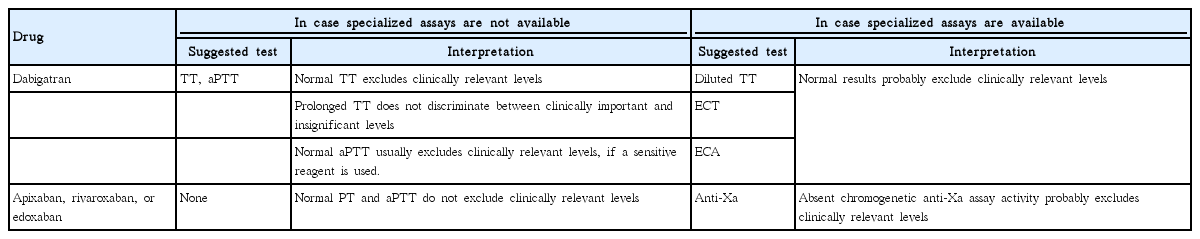
Testing of the anticoagulant activity of the varying NOACs is complex. Routine coagulation tests such as prothrombin time (PT)/international normalized ration (INR) or partial thrombin time (PTT) may be within normal limits and will only provide qualitative information. In comatose or aphasic patients OAC might go undetected unless laboratory methods such as ecarin clotting time (ECT), thrombin time (TT), factor-Xa assays are applied [10,11]. Particularly in this situation information on last intake of a NOAC may not be available. Suggestions for use of laboratory measurements and specialized assays and their interpretation are presented in Tables 1 and 2 [12,13].
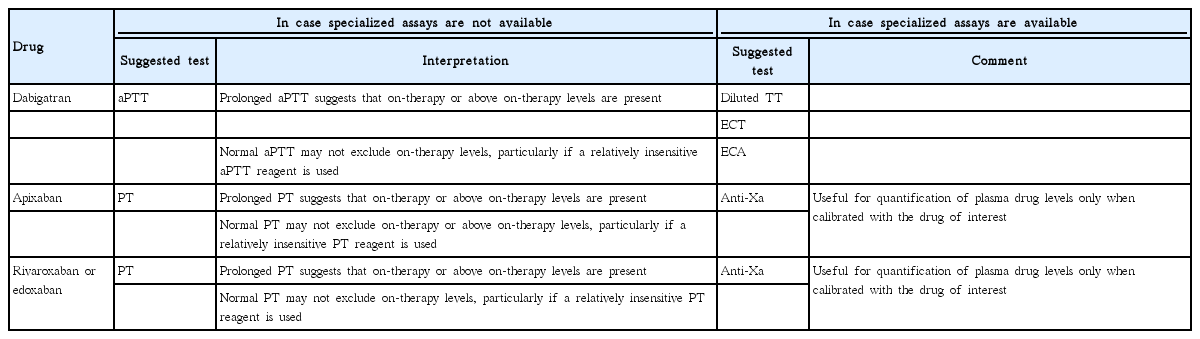
Suggestions for laboratory measurements to determine whether on-therapy or above on-therapy NOAC levels are present
Coagulation tests for factor IIa (thrombin) inhibitors (dabigatran)
The most specific tests for assessing the anticoagulant activity of dabigatran are the diluted thrombin time (dTT), the ECT, and the ecarin chromogenic assay. These tests closely correlate with dabigatran levels measured by the reference standard method, liquid chromatography-tandem mass spectrometry [12,14,15]. TT and activated partial thromboplastin time (aPTT) may be used alternatively for qualitative assessments [16]. The most sensitive test to detect the presence of dabigatran is the TT, even at very low drug concentrations. A normal-range TT assay excludes the presence of clinically relevant plasma concentrations (“clinically relevant”: NOAC levels that may contribute to bleeding or surgical bleeding risk) of dabigatran, but a prolonged TT does not discriminate between clinically important and irrelevant drug concentrations [9,12]. The aPTT is prolonged by dabigatran. But the correlation between dabigatran plasma concentrations and aPTT is non-linear. Still, a normal aPTT does not reliably exclude the presence of clinically relevant drug levels, especially when a relatively insensitive aPTT reagent is used [14,15,17]. The PT/INR is also prolonged by dabigatran but is not sensitive enough to detect clinically relevant drug concentrations.
Coagulation tests for factor Xa inhibitors (rivaroxaban, apixaban, edoxaban)
Chromogenic anti-factor Xa assays are the preferred tests for assessing the anticoagulant activity of factor Xa inhibitors, and correlate closely with plasma drug levels measured by liquid chromatography-tandem mass spectrometry [14,15]. A variety of anti-factor Xa assays correlate with plasma concentrations of rivaroxaban, apixaban, and edoxaban. All these tests must be calibrated individually for each type of therapy being assessed and are increasingly available worldwide [18]. Rivaroxaban prolongs PT/INR, with the sensitivity depending on used reagent. PT/INR may be useful for qualitative assessment of edoxaban and rivaroxaban as well, if an anti-factor Xa assay is not available (comparable to the aPTT in dabigatran) [19]. However, depending on the sensitivity of the PT reagent, a normal PT does not exclude clinically relevant levels [14,15]. A prolonged PT suggests the presence of clinically relevant apixaban levels, but a normal PT or aPTT does not exclude relevant drug levels [14,15,19]. Direct factor Xa inhibitors do not influence TT.
Point of care testing in NOAC treated patients
Point of care testing (POCT) of coagulation was proven to be of great value in accelerating emergency treatment [20]. In VKA patients the PT/INR can be measured rapidly with the CoaguChek (Roche, Basel, Switzerland), a PT/INR-POCT designed for VKA monitoring. Specific POCTs for NOACs are under investigation but not available in clinical routine yet. It was shown, that clinically relevant plasma concentrations of rivaroxaban can be qualitatively ruled out using the CoaguChek, but this method is not suitable for apixaban and dabigatran [21,22]. An INR below 1.0 (measured with CoaguChek) can rule out clinically relevant plasma concentrations of rivaroxaban (<100 ng/mL).
The Hemochron Signature (ITC, Edison, NJ, USA) is another coagulation POCT that uses a different PT/INR assay as the CoaguChek and has additional measuring capabilities for aPTT and activated clotting time (ACT) [23]. The Hemochron Signature is also responsive to rivaroxaban and dabigatran [22,24]. The diagnostic accuracy of Hemochron Signature to qualitatively rule out relevant concentrations of apixaban, rivaroxaban, and dabigatran in real-life patients was tested in a prospective observational clinical trial [23]. In this trial ACT was measured using ACT plus (ACT+) and ACT-low range (ACT-LR) test cards that contain different reagents and cover different measurement ranges. It was shown, that POCT results of PT/INR and ACT+ correlated with both, rivaroxaban and dabigatran concentrations, but only insufficiently with apixaban. So far, no convincing explanation was provided for the different reaction to the two factor Xa-inhibitors. Authors recommended the use of ACT+ test cards for rivaroxaban and PT/INR test cards for dabigatran, although both can be detected with PT/INR or ACT+ POCT cards. In conclusion, Hemochron Signature can be used to qualitatively rule out relevant concentrations of rivaroxaban and dabigatran, suggesting that this method may be a more versatile alternative for guiding emergency treatment as compared to the CoaguChek which only responded to rivaroxaban. The development of reliable POCT for all the four NOACs remains a major priority.
Managing NOAC-associated ICH
General comments on NOAC-ICH
The annual rates for ICH in NOAC treated patients is 0.23% to 0.50% [25]. The reduction of fatal bleeding in NOAC treated patients observed in RCTs and patient registries have all occurred without the availability of any specific reversal agents for the NOACs. Interestingly, a recent meta-analysis reported that the relative risk of NOACs (compared to VKAs) for fatal ICH was 0.46 (95% confidence interval, 0.36 to 0.58) without any evidence of heterogeneity across included RCTs [26]. General treatment of NOAC-ICH does not differ from treatment of spontaneous ICH and we therefore refer to ICH treatment guidelines for further information [27]. Still, we emphazise the importance of lowering systolic blood pressure: The three three large RCTs on blood pressure lowering in ICH demonstrated that intensive blood pressure lowering below systolic pressure of 140 mm Hg (above 120 mm Hg) is safe [28-30]. The latest meta-analysis demonstrates significant prevention of hematoma expansion (HE) when systolic blood pressure is lowered below 140 mm Hg [31]. The retrospective cohort study by Kuramatsu et al. [32] revealed lower rates of HE in patients with reduction in systolic blood pressure to less than 160 mm Hg within 4 hours.
Clinicians need to pay attention to comorbidities such as thrombocytopenia, uremia or liver disease, as these can worsen bleeding and subsequently outcome. Furthermore, concomitant treatments such as antiplatelet therapy need to be considered [12]. All NOACs are more or less dependent on renal function. This needs to be taken into consideration when assessing clinically relevant drug levels [33].
Bleeding classification
Bleeding complications are divided into major and non-major bleedings in clinical trials [34]. This simple categorization is also relevant in clinical routine, because major bleedings should be treated differently from non-major bleedings. The definition of a major bleeding includes a bleeding associated with hemodynamic compromise, a bleeding that occurs in an anatomically critical site, requires transfusion or results in a hemoglobin drop of 2 g/dL [12]. Critical bleeds are considered as those that compromise an organs function: the most feared is an intracranial hemorrhage [12].
Hematoma expansion in NOAC-ICH
Anticoagulation is a contributing rather than a causative factor for the occurrence of ICH. Underlying causes of OAC associated ICH and spontaneous ICH might be the same, with OAC being only a precipitating factor [35-37]. The characteristics and natural history of NOAC-associated ICH in the acute phase are largely unknown and prospective data on HE or on the effect of hemostatic management in patients receiving NOACs are limited and conflicting. The prospective registry Registry of Acute Stroke Under New Oral Anticoagulants (RASUNOA) showed that HE is frequent in NOAC-ICH (38%; in 17 of 45 subjects), has a high mortality (28% at 3 months) and an unfavorable outcome among the survivors (65%) [38]. Other observational reports and a recent meta-analysis argue that NOAC-associated ICH presents with smaller baseline hematoma volumes and lower likelihood of HE compared to VKA-ICH [39]. These observations are indirectly supported by the largest to date cohort study that compared inhospital mortality rates among patients with VKA- (n=15,036) and NOAC-ICH (n=4,918) in the Get With The Guidelines Registry. The in-hospital mortality rate was lower in NOAC-ICH (adjusted risk difference in favor of NOACs, 5.7%). This difference was further accentuated among those patients pre-treated with antiplatelet therapy in addition to OACs (adjusted risk difference in favor of NOACs, 15%) [40].
OAC reversal strategies and reversal agents
Reversal strategies for factor II Inhibitor (dabigatran) associated ICH
Idarucizumab (in early trials also called Dabi-Fab or BI 655075) has been approved 2016 as “Praxbind” in many countries for the reversal of dabigatran in patients with uncontrolled bleeding or in need for urgent emergency-procedure (Table 3). Idarucizumab is a humanized monoclonal antibody fragment that binds dabigatran with high affinity (affinity of idarucizumab for dabigatran is approximately 350 times that of dabigatran for thrombin [16]). The RE-VERSE AD (Reversal of Dabigatran Anticoagulant Effect with Idarucizumab) study, investigated dabigatran-treated patients with either ongoing severe or life-threatening hemorrhage, or in need for emergency procedures. Patients were treated with idarucizumab 5 g (2×2.5 g intravenously); the primary endpoint was the maximum reversal of the anticoagulant effect of dabigatran, which was assessed by dTT or ECT [41]. The primary endpoint was reached in 100% of the patients, and reversal was maintained for 24 hours in most patients. Concerning safety aspects, the treatment with idarucizumab was safe with no significant adverse events, especially no procoagulatory effects or complications such as venous thrombosis [41,42].
Idarucizumab should be administered as soon as the diagnosis of a dabigatran-associated ICH is proven. The results of a recently published nationwide retrospective registry reporting favorable outcomes in 12 dabigatran-associated ICH patients treated with idarucizumab further highlight the favorable therapeutic potential of this reversal agent. More specifically, rapid reversal of the anticoagulant activity was documented in all patients, hematoma growth was detected in only two cases (17%) and only one patient died during hospitalization (8%) [43].
If idarucizumab is unavailable, prothrombin complex concentrates (PCCs) have been proposed as a plausible, but unproven therapy to reverse the anticoagulant effects of NOACs, but no clinically beneficial effect of PCC was observed in dabigatran-related ICH in registries [38]. Still, based on limited data from animal, ex vivo and human studies PCC or aPCC may be administered with a dose of 50 U/kg [10,44,45]. Administration of fresh frozen plasma (FFP) or activated recombinant factor VII (rFVIIa) is not recommended for reversal of dabigatran [46].
If reversal agents are not available, diuresis with intravenous fluids may enhance renal excretion of dabigatran. Activated charcoal (50 g) may be used if the drug was ingested within last 2 to 4 hours [16]. Acute hemodialysis may be useful, because only about one-third of dabigatran is bound to plasma proteins. But hemodialysis may take too long if not started early enough [9,16].
Reversal strategies for factor Xa Inhibitor (rivaroxaban, apixaban, edoxaban) associated ICH
Andexanet alfa (r-antidote or PRT064445, “andexanet“) is a reversal agent that is designed to neutralize the anticoagulant effects of both direct and indirect factor Xa inhibitors [47]. The U.S. Food and Drug Administration approved andexanet for the use in apixaban and rivaroxaban-associated emergencies in May 2018 in the United States (Table 3) [48]. Andexanet is a recombinant modified human factor Xa decoy protein with a similar structure as endogenous factor Xa. Andexanet is catalytically inactive but retains the ability to bind factor Xa inhibitors in the active site with high affinity [49]. A bolus and 2-hour infusion of andexanet alfa rapidly reversed the anticoagulant effects of apixaban and rivaroxaban in older healthy volunteers [47]. The open-label single-group ANNEXA-4 study (NCT 02329327) evaluated andexanet in factor Xa inhibitor-treated patients with major bleeding who had taken a factor Xa inhibitor within 18 hours before start of treatment. According to an interim analysis (n=67) administration of andexanet alfa in critical bleeding resulted in effective hemostasis in 80% of patients with ICH [50]. Two different dosages and application-procedures are required for a particular factor Xa inhibitor and time since last intake (Table 3). The short half-life of andexanet alfa may be the reason for why factor Xa activity returns back to what was seen in placebo treated volunteers within 1 to 3 hours of stopping the infusion [12,47,50]. Other questions arise from a possible procoagulant effect. Until now it is unclear if observed thromboembolic events in the interim analysis were due to withheld anticoagulation or if andexanet had an impact, as andexanet binds to the natural anticoagulant tissue factor pathway inhibitor, which could produce a procoagulant effect [12,49].
Andexanet is still not widely available outside the USA and so far not approved in Europe or Asia, so that coagulation factor supplementation, e.g., with PCC or aPCC although larger scale prospective data are lacking. Serial in vivo/ex vivo experiments and animal experimental studies on the effect of PCC, aPCC, fibrinogen concentrate, or rFVIIa in NOAC demonstrated different, partially contradictory results [10]. Available clinical data on the use of four- and three-factor PCCs are conflicting. Whereas Levi et al. [51] demonstrated that three- and four-factor PCCs did have a significant normalizing effect on several coagulation tests when compared to saline, Gerner et al. [52] did not see an effect of four-factor PCC on HE in their retrospective analysis. However, the study, demonstrated a significant effect of blood pressure lowering on HE. In case of rivaroxaban, PT, and endogenous thrombin potential were completely reversed by four-factor PCC 50 IU/kg, partially by 37.5 IU/kg but not by 25 IU/kg [53]. In apixaban, partial and dose-dependent reversal was achieved by PCC 25 and 37.5 IU/kg; but data on 50 IU/kg are not available [54]. In edoxaban, full reversal was achieved by 50 IU/kg and partially by 10 and 25 IU/kg [55].
Concerning dosing of four-factor PCCs EHRA-guidelines recommend a dose of 50 U/kg [56]. As there are no randomised data regarding dosing in factor Xa inhibitor treated patients with major bleeding, a dose of 50 U/kg is also recommended for aPCC, instead of the higher dosing up to 100 U/kg typically administered in hemophilia patients [12,57]. APCC may be more potent but also have higher thrombogenic potential [58].
As there is no sufficient evidence for FFP, plasma should not be administered in the setting of FXa-associated ICH. Due to a higher thromboembolic risk of rFVIIa compared to PCC, rFVIIa can be administered, but it is recommended to prefer PCC as nonspecific reversal strategy [46]. We recommend not to use rFVIIa.
In case PCC is not available or is not suitable, administration of activated charcoal (50 g) may be considered. Dialysis is not suitable for factor Xa inhibitors because of high plasma protein binding (85% to 95% for apixaban and rivaroxaban, 65% for edoxaban). Therefore, plasmapheresis seems more plausible in these cases [11], but is only reasonable if applied shortly after intake of the drug.
Reversal agents under development
Another target-specific reversal agent in clinical proving is ciraparantag (also called PER977, aripazine), a small synthetic molecule, that might reverse the activity of all NOACs—both the factor Xa and factor IIa inhibitors—as well as certain forms of heparin [59]. The water-soluble cationic molecule binds via a noncovalent charge-charge interaction to direct and indirect inhibitors of factor Xa and thrombin and prevents the anticoagulant from binding to its endogenous target once it is bound [60]. Ciraparantag is still in the early stages of development and several phase II studies for the different NOAC are currently conducted (NCT01688830 or NCT02104947 (dabigatran); NCT017 58432 (rivaroxaban and apixaban). For edoxaban (NCT01826266) the study demonstrated rapid and maintained (24 hours) reversal of whole-blood clotting times in 80 volunteers [60,61]. In an in vivo study on rat-tail–transection bleeding assays ciraparantag reversed anticoagulation with each of the new oral agents and did not bind to plasma proteins, including albumin, no procoagulant effects have been identified. Adverse effects were flushing symptoms and dysgeusia [60]. To our knowledge there is no phase III trial conducted, so that approval of this potential reversal agent remains speculative.
Finally, modified thrombin molecules as specific reversal agent for dabigatran have been investigated. Genetically changed and therefore inactive or trypsinized thrombin molecules (S195A-IIa or γT-S195AIIa) could antagonize the anticoagulative effect of dabigatran in an in vivo analysis and in a mouse model [62]. There are no clinical data available for this reversal agent.
Considerations for restarting anticoagulation
For a long time, ICH has been considered as contraindication for further anticoagulation. The risk of recurrent ICH while on OAC was assumed double as high as with the overall recurrence risk of ICH. The mortality rate associated with recurrent ICH can be as high as 50% [63,64]. On the other hand there is the high risk of systemic and cerebral embolism in patients with NAF. Data concerning this conflicting issue are rare and personal opinion generally shapes the decision. Furthermore, the labels of the NOAC state that ICH constitutes a contraindication for OAC and therefore re-starting anticoagulation after ICH would be off-label use. The decision on restarting OAC means to balance between two risks: ischemic stroke and rebleeding and is often made on the basis of a risk-benefit analysis for the individual patient [9,65]. In most cases there is net clinical benefit in favor of restarting OAC after an ICH if there is a proven indication for OAC [66], and especially in patients with deep hemispheric ICH [63,67,68]. In a German retrospective cohort study OAC was resumed in 23.9% of VKA-ICH survivors. There were fewer cerebral ischemic events and no difference in recurrent ICH in patients who received OAC after an ICH compared to those who did not. Furthermore, OAC resumption was significantly related to a decreased long-term mortality [32]. The individual patient data meta-analysis of the three cohorts (including the German) confirmed these results and revealed that there are no differences between patients with lobar and deep ICH and also not between patients with possible and probable cerebral amyloid angiopathy [69]. An analysis of Danish registries also found a significant reduction in ischemic stroke and mortality in post-ICH anticoagulated patients [70,71].
The relative reduced risk of ICH with NOACs compared to warfarin renders NOACs the preferred drugs when resuming OAC after ICH. However, data from a prospective randomised phase II trial (APACHE-AF trial, NCT02565693, clinicaltrials.gov) investigating this for apixaban are not available yet. For dabigatran an observational study showed, that resumption of OAC with either dabigatran or warfarin after a major bleeding event was associated with increased survival and stroke-free survival compared with discontinuing anticoagulation. In addition, dabigatran was associated with lower risk of recurrent hemorrhage than warfarin [66]. Physicians should consider the availability of a NOAC-specific reversal agent when selecting the NOAC agent for resuming anticoagulation in patients with prior NOAC-ICH.
Suggested factors that contribute to the risk-benefit assessment of restarting anticoagulation are patient’s age, renal function (with worsening of renal insufficiency leading to elevated OAC levels), the location of ICH, presence of the apolipoprotein Ɛ2 or Ɛ4 alleles, and greater number of cerebral microbleeds on MRI [9]. In the meantime, physicians might consider whether left atrial appendage occlusion is an option in selected patients with an increased bleeding risk due to the prior NOAC-associated ICH [71-74].
The optimum timing of the resumption of anticoagulation is another challenge with conflicting evidence. Lower rates of ischemic strokes can already be observed at 2 weeks in patients who were restarted on OAC compared to those who were not in the geRman-widE mulTicenter Analysis of oRal Anticoagulation-associated intraCerebral hEmorrhage (RETRACE) study [32]. These data were not available when the current American Heart Association were already published in 2015. They advocate avoidance of oral anticoagulation for at least 4 weeks, in ICH patients without mechanical heart valves and indication of anticoagulation (Class IIb/Level of Evidence B recommendation) [75]. We propose to restart NOAC not earlier than 2 to 4 weeks after ICH, taking into consideration the aforementioned risk factors and particularly blood pressure, as anticoagulation should not be re-started in patients with elevated blood pressure and a clear indication for OAC. We also advocate to include patients in RCTS (e.g., APACHE-AF trial, NCT02565693, clinicaltrials.gov) whenever possible.
Conclusions
Although mortality in ICH has been reduced during the last decades and NOACs appear to have a better safety profile compared to VKAs, oral anticoagulant therapy-ICH is frequent and treatment challenging. Physicians should be aware, that restoring coagulation and lowering blood pressure as soon as possible are crucial in order to prevent HE. More available coagulation tests for NOACs and POCTs for emergency situations may help to manage these patients in future. Further investigations are warranted concerning reversal agents, which will hopefully lead to a reduction of mortality and disability of these critically ill patients.
Notes
Disclosure
Thorsten Steiner received speaker fees and consultations fees from Boehringer-Ingelheim, Bayer, BMS Pfizer, and Daiichy Sankyo. Peter D. Schellinger has received speaker and consultation fees from Boehringer-Ingelheim, Bayer, BMS Pfizer, and Daiichy Sankyo. Georgios Tsivgoulis has received speaker and consultation fees from Boehringer-Ingelheim, Bayer, and Daiichy Sankyo.
Acknowledgements
We thank Corinna Epple for her contribution to the content of the article.