 |
 |
- Search
| J Stroke > Volume 22(2); 2020 > Article |
|
Dear Sir:
The coronavirus disease of 2019 (COVID-19) pandemic has caused significant stress to the healthcare practice. Ischemic stroke was observed in 2.3% hospitalized COVID-19 patients and 4.5% patients with severe COVID-19 infections [1]. In this letter, we report a ŌĆ£modified code strokeŌĆØ in the management of hyperacute stroke under the COVID-19 crisis followed in a tertiary medical center in Taiwan.
The Taiwan Central Epidemic Command Center (CECC) has coordinated nationwide preventive strategies to intercept the spread of COVID-19. Besides laboratory confirmed COVID-19 cases, the CECC has defined three risk levels for COVID-19 infection [2]. People having unprotected contact with confirmed COVID-19 patients or travelling from abroad within the past 14 days are either home-isolated or quarantined and tested for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), if symptoms developed. Patients with pneumonia, and high-risk social status (medical workers, pulblic transport workers, history of joining public gathering) with symptoms of fever, respiratory tract infection, anosmia, and/or dysgeusia are tested for SARS-CoV-2 as community-based surveillance. Till April 18, 2020, 52,445 SARS-CoV-2 reverse-transcription polymerase-chain reaction (RT-PCR) tests were performed in Taiwan, of which 343 were confirmed COVID-19 cases, 333 were included in the 14,151 tests of patients at airports or under home isolation/quarantine (positive rate 2.3%), and 10 were included in the 38,294 tests of community-based surveillance (positive rate 0.026%). The risk of community transmission was considered low.
The National Cheng Kung University Hospital (NCKUH) is a 1,320-bed tertiary medical center in Southern Taiwan. Figure 1 summarizes the ŌĆ£modified code strokeŌĆØ followed in the NCKUH, and the strategies are summarized in Supplementary Table 1. Patients used to be treated using the standard code stroke (Supplementary methods [3-5]) are treated using the ŌĆ£modified code strokeŌĆØ and transported to the negative-pressure isolation room if their clinical infection screen based on exposure history and/or symptoms result in positive or poor-quality. All medical personnel in close proximity with the patients wear personal protective equipment to prevent air, droplet, and/or contact infection [6]. The patients wear surgical masks throughout the ŌĆ£modified code stroke.ŌĆØ
We use the modified National Institutes of Health Stroke Scale (NIHSS) to evaluate the severity of stroke. To avoid the removal of patientsŌĆÖ surgical masks, we score 1 point for facial palsy if the patient has mild dysarthria, and 2 points if the dysarthria is moderate to severe. The finger-nose-finger test is substituted with the finger-to-nose test to decrease contact exposure. Before neurological evaluation, a nasopharyngeal swab is obtained early from the patient and screened for SARS-CoV-2 by RT-PCR, to promote hemostasis of the swabbed site before potential thrombolysis treatment. While obtaining the nasopharyngeal swab, the patientŌĆÖs surgical mask is displaced inferiorly to expose the nostril, but it covered the patientŌĆÖs mouth to minimize the possibility of droplet spread.
After clinical evaluation, the patient is transported to the computed tomography (CT) room through a special corridor that ensures a distance of at least 1.5 m between the patient and other people. The air conditioning of the CT room is turned off throughout the examination and is turned on after surface decontamination and disinfection with ultraviolet light. Noncontrast chest CT is performed to evaluate the presence of pneumonia. The choice of brain scan depends on the potential need for endovascular thrombectomy (EVT), determined clinically by NIHSS, signs of large vessel occlusion, and risk of COVID-19, as discussed later.
After clinical and radiographic evaluations, we assess the risk of COVID-19. Patients with confirmed COVID-19, under home-isolation or quarantine, or with evidence of pneumonia on chest CT are considered as high risk of COVID-19. Patients with high-risk social status accompanied by fever and symptoms of respiratory tract infection are considered as intermediate risk of COVID-19. The remaining are considered as low risk of COVID-19. Patients with low risk are released from the isolation to be treated by the standard code stroke. Patients with high or intermediate risk are transferred to the negative-pressure isolation room. The eligibility and protocol of intravenous thrombolysis are same as in standard code stroke.
Taiwan Stroke Society suggested that the risk of infectious exposure in medical workers treating patients with high risk of COVID-19 should be considered [7] due to limited number of neuro-interventionists and lack of negative-pressure angiography rooms in Taiwan. In NCKUH, we excluded patients with high risk of CIVID-19 from EVT in ŌĆ£modified code stroke.ŌĆØ
Patients with intermediate risk of COVID-19 can undergo ŌĆ£protected EVTŌĆØ if eligible. These patients are intubated in the negative-pressure isolation room [8], and an endotracheal tube is connected to a portable ventilator and closed sputum-suction system. During the procedure, the angiography room is under positive pressure as usual. The patient is under conscious sedation, and ventilation is supported by the portable ventilator to avoid disconnection of the closed respiratory system. After the procedure, the same disinfection procedures as the CT room are performed.
After hyperacute treatment, the patient is admitted to a negative-pressure room or single room in the intensive care unit (ICU). All patients with intravenous thrombolysis and EVT are advised follow-up brain CT 24 hours after treatment. We conduct the SARS-CoV-2 RT-PCR tests every 24 hours. Confirmed patients with COVID-19 are released from isolation only after three consecutive negative results. Home-isolated/quarantined patients are released after two consecutive negative results. Patient under community-based surveillance are released after negative initial test results. Brain MRI is performed after the patientŌĆÖs release.
This protocol can be further modified in the future. First, EVT in patients with high risk of COVID-19, especially in home-isolated/quarantined patients, can be re-initiated if a reliable, high-sensitivity, rapid test of SARS-CoV-2 is developed. Second, training emergency medical technicians in the pre-hospital notification of code stroke can minimize the time required for in-hospital preparation. Third, if all ICU beds are occupied by critical cases, early step-down transfer may be reasonable [9]. Finally, evidence regarding the influence of COVID-19 on stroke and hyperacute stroke treatment is limited [10]. Further studies are warranted, and new evidence will further change the ŌĆ£modified code stroke.ŌĆØ
Supplementary materials
Supplementary materials related to this article can be found
online at https://doi.org/10.5853/jos.2020.01599.
Supplementary┬ĀTable┬Ā1.
Summary of strategies in the modified code stroke
Acknowledgments
This work received a grant from the National Cheng Kung University Hospital (Grant number: NCKUH-20200062).
We thank the Stroke Center, Center for Infection Control, Department of Emergency Medicine, Department of Medical imaging, and Department of Anesthesiology at the National Cheng Kung University Hospital in helping us to design this modified protocol. We thank the National Cheng Kung University Hospital for funding this work.
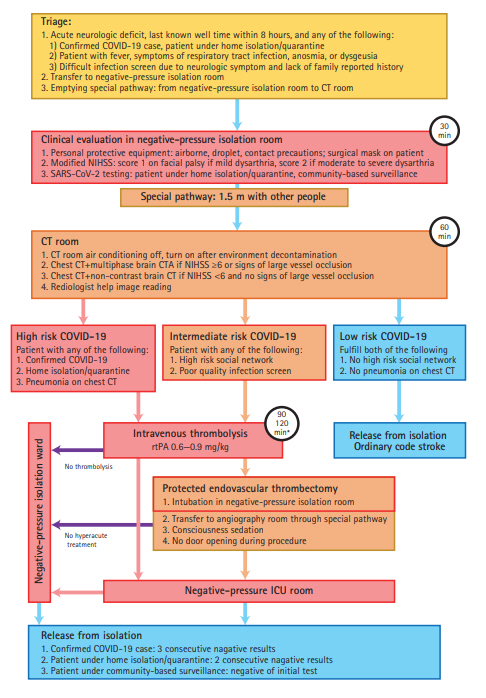
Figure┬Ā1.
Modified stroke protocol in the National Cheng Kung University Hospital, Taiwan. The box with red rim indicates negative-pressure isolation environment. The box with orange rim indicates environments with modifications in ventilation. The box with yellow rim represents medical staff wearing personal protective equipment. The goal is achieve a door-to-needle time for intravenous thrombolysis as 90 minutes, if non-contrast brain computed tomography (CT) is performed and 120 minutes, if multiphase CT angiography is performed. COVID-19, coronavirus disease of 2019; CTA, computed tomography angiography; NIHSS, National Institutes of Health Stroke Scale; SARS-CoV-2, severe acute respiratory syndrome coronavirus 2; rtPA, recombinant tissue plasminogen activator; ICU, intensive care unit. *90 minutes if non-contrast CT, 120 minutes if multiphase CTA.
References
1. Mao L, Jin H, Wang M, Hu Y, Chen S, He Q, et al. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol 2020;Apr. 10. [Epub]. https://doi.org/10.1001/jamaneurol.2020.1127.


2. Taiwan Central Epidemic Command Center. CECC measures for following up on persons at risk of infection. Taiwan Centers for Disease Control; https://www.cdc.gov.tw/En/File/Get/Bj-bAcC0SN3kVWwG1gKWxA. 2020. Accessed May 14, 2020.
3. Tang SC, Tsai LK, Chen CJ, Lee CW, Wang KC, Lai YJ, et al. 2019 Taiwan Stroke Society guideline for endovascular thrombectomy in acute ischemic stroke patients. Formos J Stroke 2019;1:77-89.
4. Chen CH, Hsieh HC, Sung SF, Hsieh CY, Chen PL, Tsai LK, et al. 2019 Taiwan Stroke Society guideline for intravenous thrombolysis in acute ischemic stroke patients. Formos J Stroke 2019;1:1-22.
5. Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, et al. Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2019;50:e344-e418.


6. Taiwan Centers for Disease Control. Interim guidelines for clinical management of SARS-CoV-2 Infection (5th edition) Taiwan Centers for Disease Control; https://www.cdc.gov.tw/En/File/Get/_Dv_q75ZjLcNeRvlnrPgUg. 2020. Accessed May 14, 2020.
7. Chen CH, Liu CH, Sung PS, Hsieh CY. Taiwan Stroke Society recommendations for hyperacute stroke management during the COVID-19 pandemic. Formos J Stroke 2020;2:1-4.
8. Fraser JF, Arthur AS, Chen M, Levitt M, Mocco J, Albuquerque FC, et al. Society of NeuroInterventional Surgery recommendations for the care of emergent neurointerventional patients in the setting of covid-19. J Neurointerv Surg 2020;Apr. 15. [Epub]. https://doi.org/10.1136/neurintsurg-2020-016098.

9. Temporary emergency guidance to US stroke centers during the COVID-19 pandemic. Stroke 2020;Apr. 1. [Epub]. https://doi.org/10.1161/STROKEAHA.120.030023.








