 |
 |
- Search
| J Stroke > Volume 23(1); 2021 > Article |
|
Dear Sir:
The first pass effect (FPE) is an independent predictor of good functional outcomes (modified Rankin Scale [mRS] 0-2) and is associated with reduced 90-day mortality [1]. However, the economic impact of FPE has not been evaluated in the Asia-Pacific (APAC) region. This analysis assessed the procedural/hospitalization-related and long-term care economic impact of achieving FPE in patients with acute ischemic stroke in Australia, India, Japan, South Korea, Singapore, and Taiwan.
A detailed description of the methods can be found in Supplementary methods. Briefly, post hoc analyses were conducted using patient-level data from the 227 patients in the Analysis of Revascularization in Ischemic Stroke With EmboTrap (ARISE) II study, a prospective single-arm international multi-center clinical trial investigating the efficacy and safety of the EmboTrap device (Cerenovus, Irvine, CA, USA) [2]. FPE was defined as restoring complete or near complete reperfusion (modified Thrombolysis in Cerebral Infarction [mTICI] 2c-3) in a single pass with the EmboTrap device. The target population comprised patients who achieved mTICI 2c-3 (n=172), stratified into two groups: FPE (mTICI 2c-3 after the first pass) and non-FPE (mTICI 2c-3 after multiple passes). Primary analyses were conducted in two steps. First, clinical and healthcare resource use data from the ARISE II study were evaluated for the FPE and non-FPE groups. Second, cost data from peer-reviewed literature or market research (Supplementary Table 1) were applied to healthcare resource use data from the ARISE II study to assess cost consequences in each group using two time-horizons to accommodate two different perspectives: (1) procedural/hospitalization-related (i.e., length of stay [LOS], standard bed days, intensive care unit [ICU] days, and procedural devices used) assessing costs from the healthcare provider perspective; and (2) long-term care costs based on 90-day mRS (per annum for Australia, Japan, and South Korea; 6 months for India) assessing costs from the payer perspective. All costs were reported as 2020 currencies or 2020 United States dollar (USD) except Singapore (2019 currencies) and were inflated using country-specific inflation indices. Sensitivity analyses, varying key input parameters (i.e., alternative definitions for FPE [“FPE, mTICI 3” and “FPE, mTICI 2b-3”], LOS, healthcare resource costs, and inclusion of costs for mRS 6), were conducted to test the robustness of the results.
Complete or near-complete reperfusion (mTICI 2c-3) was observed in 76% of the patients (n=172) in the ARISE II study. Among patients that achieved mTICI 2c-3, 53% (n=91) achieved FPE. Baseline characteristics were balanced between the FPE and non-FPE groups (Supplementary Table 2). Patients in the FPE group had better clinical outcomes (Supplementary Table 3). Furthermore, patients who achieved FPE required a single EmboTrap device whereas 35% of patients in the nonFPE group required additional devices such as other stent retrievers and/or aspiration catheters. Patients in the FPE group had a significantly shorter mean LOS (6.10 days [interquartile range (IQR), 3.00 to 8.00] vs. 9.48 days [IQR, 3.00 to 11.00], P<0.01) and spent significantly fewer mean number of days in a standard bed (3.05 [IQR, 0.00 to 5.00] vs. 6.13 [IQR, 1.00 to 8.00], P<0.01). The mean number of days spent in the ICU (3.39 [IQR, 2.00 to 4.00] vs. 3.58 [IQR, 2.00 to 4.00], P=0.70) was similar between groups. Achieving FPE led to estimated perpatient procedural/hospitalization-related cost savings in every country studied (8,621 Australian dollar [AUD] or $5,951 USD for Australia, 67,718 Indian rupee [INR] or $894 USD for India, ¥239,493 or $2,241 USD for Japan, ₩2,004,146 or $1,655 USD for South Korea, 5,544 Singapore dollar [SGD] or $3,981 USD for Singapore, and 41,911 Taiwan dollar [TWD] or $1,416 USD for Taiwan) (Figure 1). Similarly, achieving FPE led to estimated per-patient long-term care cost savings in every country studied (398 AUD or $275 USD for Australia, 68 INR or $1 USD for India, ¥314,262 or $2,941 USD for Japan, and ₩6,155,006 or $5,084 USD for South Korea) (Figure 2). Results from the sensitivity analyses were consistent with the primary analyses; notably, inclusion of costs for mRS 6 resulted in long-term care cost savings of 13,353 INR for India and ₩8,359,695 for South Korea (Supplementary Table 4).
This study demonstrated that achieving FPE led to potential per-patient procedural/hospitalization-related cost savings, which is especially meaningful for healthcare systems that pay hospitals on the basis of diagnosis-related groups or related payment models. These potential cost savings were largely driven by improvements in clinical outcomes; research has shown that increases in mean LOS are directly correlated with mRS evaluated 90 days after a stroke [3]. The potential long-term care cost savings from improvements in functional outcomes are linked to reduced healthcare resource use and decreased costs for patients surviving stroke [4]. Our findings are aligned with a cost-effectiveness analysis that showed that achieving expanded Thrombolysis in Cerebral Infarction (eTICI) 3 resulted in more quality-adjusted life years, as well as healthcare and societal cost savings compared with achieving eTICI 2b among patients with large vessel occlusions [5].
There are several factors related to the treating physician (e.g., training), setting (e.g., available equipment), and patient (e.g., clot composition) that may impact the ability to achieve FPE; however, techniques involving the combined use of stent retrievers and other devices (e.g., intermediate catheters) may improve recanalization rates and the rate of FPE [6,7]. As such, it may be beneficial to use techniques involving multiple devices immediately rather than beginning with a single device approach and gradually combining additional devices to achieve reperfusion after initial failure.
This study had some limitations. First, healthcare resource use collected from clinical trials may not reflect the real-world setting. It is plausible that costs calculated from ARISE II resource utilization may be different in Asia due to variations in clinical practice or population-specific factors. Although sensitivity analyses assessing differences by ethnic groups/regions were considered, such analyses were not feasible due to small sample sizes. Second, the ARISE II study did not report cost data; as such, costs were obtained from peer-reviewed literature or market research, limiting validity. However, this study used the best available estimates, which were validated by clinical experts in interviews.
In conclusion, achieving FPE led to potential procedural/hospitalization-related and long-term care cost savings in the APAC region in addition to clinical benefits. As such, achieving reperfusion with a single pass is a relevant goal for endovascular treatment of acute ischemic stroke with holistic benefits.
Supplementary materials
Supplementary materials related to this article can be found online at https://doi.org/10.5853/jos.2020.05043.
Acknowledgments
This study was funded by Cerenovus, a subsidiary of Johnson and Johnson.
Leonard Yeo is a consultant for Stryker and See-mode. Leonard Yeo has equity in Cereflo; Osama O. Zaidat is a consultant for Neuravi, Stryker, Penumbra, and Medtronic; Jeffrey L. Saver is an employee of the University of California, which holds a patent on retriever devices for stroke. The University of California, Regents receives funding for Jeffrey L. Saver’s services as a scientific consultant regarding trial design and conduct to Covidien/Medtronic and Stryker. Jeffrey L. Saver serves as a consultant (modest) for Abbott, Medtronic, Stryker, and Neuravi/Cerenovus. Jeffrey L. Saver also has contracted stock options (modest) for Rapid Medical; Heinrich P. Mattle reports personal fees from Covidien/ Medtronic, personal fees from Neuravi/Cerenovus, personal fees from Servier, and personal fees from Bayer outside the submitted work; served on the steering committees of the SWIFT PRIME and ARISE studies; Stephanie Hsiao Yu Lee and Emilie Kottenmeier are employees of Johnson and Johnson; Heather L. Cameron and Rana A. Qadeer are paid consultants for Cerenovus; Tommy Andersson is a consultant for Neuravi/Cerenovus, Anaconda, Amnis Therapeutics, and Rapid Medical; served on the steering committees of the ARISE studies.
Figure 1.
Estimated per-patient procedural and hospitalization-related healthcare use cost savings for the first pass effect (FPE) and non-FPE groups. Negative values represent cost savings for patients in the FPE group as compared with the non-FPE group. Numbers may not sum due to rounding. AUD, Australian dollar; INR, Indian rupee; SGD, Singapore dollar; TWD, Taiwan dollar; LOS, length of stay; USD, United States dollar. *Reported as charges; †Reported as 2019 USD for Singapore. Exchange rates reported for June 22, 2020 16:00 Coordinated Universal Time (UTC) were used for all countries. The exchange rates were as follows: 1.00 AUD:0.69 USD; 1.00 INR:0.01 USD; 1.00 JPY:0.01 USD; 1.00 ₩:0.001 USD; 1.00 SGD:0.72 USD; and 1.00 TWD:0.03 USD.

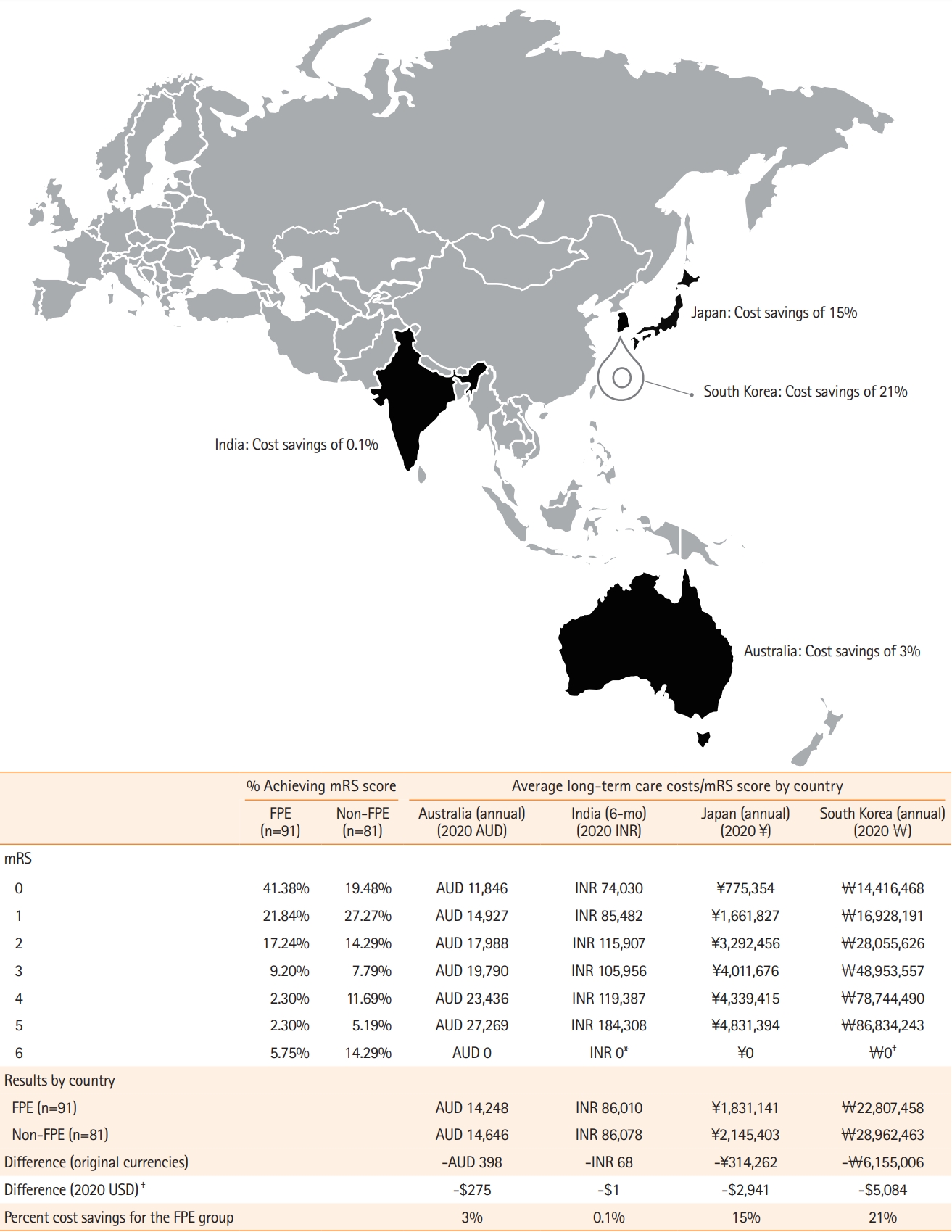
Figure 2.
Estimated per-patient long-time care cost savings, based on 90-day modified Rankin Scale (mRS), for the first pass effect (FPE) and non-FPE groups. Negative values represent cost savings for patients in the FPE group as compared with the non-FPE group. Numbers may not sum due to rounding. AUD, Australian dollar; INR, Indian rupee; USD, United States dollar. *Reported for India and South Korea but not used for analyses to ensure consistency with other countries that did not report a cost for death (i.e., mRS 6); †Exchange rates reported for June 22, 2020 16:00 Coordinated Universal Time (UTC) were used for all countries. The exchange rates were as follows: 1.00 AUD:0.69 USD; 1.00 INR:0.01 USD; 1.00 JPY:0.01 USD; and 1.00 ₩:0.001 USD.
References
1. Zaidat OO, Castonguay AC, Linfante I, Gupta R, Martin CO, Holloway WE, et al. First pass effect: a new measure for stroke thrombectomy devices. Stroke 2018;49:660-666.


2. Zaidat OO, Bozorgchami H, Ribó M, Saver JL, Mattle HP, Chapot R, et al. Primary results of the multicenter ARISE II study (Analysis of Revascularization in Ischemic Stroke With EmboTrap). Stroke 2018;49:1107-1115.

3. Dawson J, Lees JS, Chang TP, Walters MR, Ali M, Davis SM, et al. Association between disability measures and healthcare costs after initial treatment for acute stroke. Stroke 2007;38:1893-1898.


4. Lobotesis K, Veltkamp R, Carpenter IH, Claxton LM, Saver JL, Hodgson R. Cost-effectiveness of stent-retriever thrombectomy in combination with IV t-PA compared with IV t-PA alone for acute ischemic stroke in the UK. J Med Econ 2016;19:785-794.


5. Kunz WG, Almekhlafi MA, Menon BK, Saver JL, Hunink MG, Dippel DWJ, et al. Public health and cost benefits of successful reperfusion after thrombectomy for stroke. Stroke 2020;51:899-907.










